Thanks to eDerm’s Smart Coding™ feature – billing and coding have never been easier. Here are some of the key features that make our SmartCoding™ feature so easy to work with:
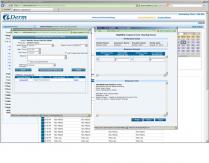
E&M Calculator
Our EHR for dermatologists uses an industry standard method of billing for your office visit CPT. Our E&M Calculator assesses your current level and tells you what additional activities you can do to reach the next level.
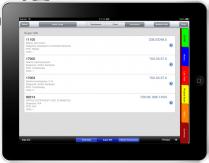
Super Bill
Within our EMR dermatologists can view a Super Bill. eDerm automatically creates and displays a Super Bill within the iPad app summarizing the encounter including all the ICD9/ICD10 diagnoses along with the CPT procedure code performed for each problem. It also gives you the flexibility to make changes. On the Super Bill, you may edit the ICD9/ICD10s and add new ICD9/ICD10 to CPT mappings.
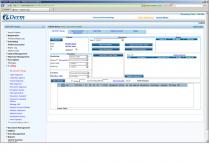
Impression Details
The integrated functionality within the eDerm system makes the entire coding process seamless. In the impression details, eDerm provides ICD9/ICD10 code editing – that means it will automatically remember how you like to code each impression and carry these codes over to the Super Bill.
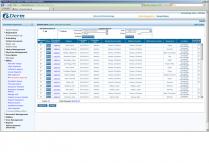
CPT Coding
Not all CPTs are generated in the same way. Some are specific to quantities and/or locations. So eDerm automatically tracks quantities and locations to code the specific CPTs to the correct values.